|
To protect itself, the Leishmania parasites have developed different mechanisms to protect itself against host defenses, such as:
Previous studies have shown the possibility that acquisition of drug resistance could affect the fitness of the parasites, influencing properties involved in parasite proliferation. Researchers then decided to evaluate whether L. donovani lines, which are experimentally resistant to single anti-leshmanial drugs or to a combination of drugs, could have an advantage over susceptible cells in tolerating stress conditions. Researchers placed resistant and susceptible cell lines under different stress conditions, and recorded the growth of the cell lines, using Luciferase as an indicator of parasite proliferation. The stress conditions the cell lines were placed under were:
resultsIn the absence of nutritional stress, neither the resistant nor the susceptible cell lines showed any significant advantage over the other. However, during the late stationary phase assay, it was observed that resistant cell lines had higher growth rates than the susceptible cells, probably due to a higher resistance to stress conditions that were present during the stationary stage. Similarly, under starvation conditions, resistant cell lines, more specifically those resistant to a combination of drugs, demonstrated an advantage over susceptible cell lines in the absence of nutrients. The higher survival rates of resistant cell lines were probably due to their ability to adapt their metabolism to handle the stress of starvation. Under heat shock and pH stress, resistant cell lines once again demonstrated higher tolerance against such conditions compared to susceptible cell lines. This suggests that resistant strains could demonstrate a higher survival rate inside hosts during their life cycle. conclusionLeishmania cell lines that were experimentally resistant to single or combination of anti-leishmanial drugs have exhibited an advantage over susceptible cell lines in terms of fitness, presumably due to a higher tolerance to stress conditions. Therefore, if such drug-resistant parasites were to be spread around in the environment, it could pose problems towards strategies to control the disease, such as chemotherapy.
References:
0 Comments
Research has shown yet another component in our body's immune system that could prove vital in controlling Leishmaniasis. This time, our body's memory T cells are the main players in controlling this terrible condition.  So far, it is understood that after a VIRAL infection, memory T cells are formed, which will result in a quicker and more effective immune response during a reinfection by the virus. A new study has shown that the same mechanism also applies after a PARASITIC infection, opening new doors in research for ways to combat and control Leishmaniasis, amongst other diseases. There are 2 kinds of T cells, CD4 and CD8 T cells. CD4 T cells assist in the immune response by activating other immune cells, while CD8 T cells are able to kill pathogens directly. Following an infection, a population of T cells that survive become memory T cells, which circulate around the body. However, it is suspected that these circulating memory T cells are not the only way the body protects against immunity... After transferring CD4 T cells from a mouse that has recovered from Leishmaniasis to another mouse who has never contracted the disease, it was observed that the latter only received PARTIAL protection, which led researchers to suspect another element was missing from the equation. By observing more mice who had recovered from Leishmaniasis, researchers discovered parasite-specific T cells in the skin, not only from the site of infection, but other sites as well. Further studies showed that these T cells were unlike the memory T cells which circulated around the body after an infection, they were actually residents of the skin! These resident CD4 memory T cells are also able to recruit other T cells to the site of infection, a key process in fighting off infections.
Mice that received tissue-resident CD4 cells via a skin graft from mice previously infected with Leishmaniasis, when given an injection of Leishmania-responsive T cells, were able to respond to an infection as effectively as a mouse that has developed natural immunity. This hints at a possibility of a vaccine through a method similar to that of the Smallpox vaccine, via a process known as scarification, which involves scratching the skin. This effectively generates tissue-resident memory cells. There has been extreme difficulty treating patients positive for both visceral leishmaniasis and HIV. Both diseases affect the immune system of the patients and are fatal if left untreated. As if tackling a single disease isn't enough, now patients would have to deal with 2! The risk of death for patients with visceral leishmaniasis co-infected with HIV is 9x higher. Visceral leishmaniasis also causes the progression of HIV to speed up, and relapses of the disease is more common in patients co-infected with HIV. Chances of curing visceral leishmaniasis are also significantly lower. A study in India treated patients with confirmed visceral leishmaniasis-HIV co-infections with a combination of drugs, amphotericin B and miltefosine, and encouraged to start on antiretrovial therapy.
102 patients were followed-up for an average of 11 months, and from the results of the study, combination therapy appeared to be a safe and effective way for treatment of visceral leishmaniasis in HIV co-infected individuals. Inflammasomes are important structures of our immune system in combating pathogens. Their effect on bacterial and viral pathogens are well studied, while in contrast, their effect on protozoan parasites, such as Leishmania, are less studied [1]. However, research led by scientists at St. Jude Children Hospital have led to surprising revelations about resistance against Leishmaniasis. Studies were carried out on mice infected with Leishmaniasis. As part of the body's immune response, NLRP3 inflammasomes sense Leishmania parasites and produce interleukin 18 (IL-18), messenger molecules involved in the body's first line of defence against diseases. Surprisingly, inhibiting IL-18 protected specially bred mice from the most common form of Leishmaniasis instead of aggravating the disease. Scientists had expected, based on previous studies with a different mouse model of Leishmaniasis, for IL-18 to induce an immune response, resulting in production of molecules involved in protection against Leishmaniasis. However, the opposite happened, and IL-18 induced the production of interleukin 4 (IL-4), which skewed the immune response in the parasite's favour instead [2]. Thus, by inhibiting NLRP3 inflammasomes, IL-18 production declined and the mice were resistant towards the infection. In conclusion, neutralizing IL-18 protected mice against Leishmaniasis, suggesting that the same might be able to be done for humans.
The Islamic State of Iraq and Syria (ISIS), notorious throughout the world for the acts of terrorism against women and other religions, faces an unseen threat, literally. Leishmaniasis, a disease caused by the protozoan parasite Leishmania, has been spreading through the ranks of ISIS soldiers in the Middle East. These parasites can be carried and transmitted by sand flies, which are commonly found in sandy environments. It can be further aggravated by poor hygiene and pollution. There are 3 different forms of the disease, with the most common being cutaneous, which may developed into visceral leishmaniasis if left untreated. The other form is mucocutaneous, which causes ulcers in the skin, mouth, and nose. 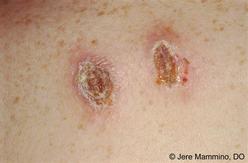 Leishmaniasis causes the skin or mucosal membranes to develop lesions and sores, appearing as it the flesh has been eaten. Left untreated, it may eventually lead to death. According to medical reports, more than 100,000 cases have been reported among ISIS fighters, with numbers expected to climb as they are not seeking medical treatment. In addition, as ISIS is an organization dedicated to terrorism, it is unlikely that they will receive medical attention as well. Luckily for us, the disease only affects a small area, as 90% of all reported cases were found in only 6 countries: Bangladesh, Brazil, Ethiopia, India, South Sudan, and Sudan. References:
|
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
August 2015
Categories |

 RSS Feed
RSS Feed
